Endothelial Dysfunction and Atherosclerosis
Dicken Weatherby, N.D. and Beth Ellen DiLuglio, MS, RDN, LDN
Damage to the endothelium is the first step on the road to full blown atherosclerosis, which contributes to most heart attacks and strokes.[1] Because atherosclerosis causes ischemic heart disease, it is, in fact, considered the main cause of death around the world.
The Endothelial Dysfunction Series
- Endothelial Dysfunction - An Overview
- Endothelial Dysfunction - The Endothelium
- Endothelial Dysfunction - Nitric Oxide
- Endothelial Dysfunction - Diseases and Causes
- Endothelial Dysfunction - Immune Response & Oxidative Stress
- Endothelial Dysfunction & Atherosclerosis
- Endothelial Dysfunction - Assessment Part 1
- Endothelial Dysfunction - Assessment part 2
- Endothelial Dysfunction - Functional Naturopathic Approach
- Endothelial Dysfunction - The Optimal Takeaways
Atherosclerosis is characterized by:[2]
-
Endothelial dysfunction
-
Vascular inflammation
-
Buildup of lipids, cholesterol, calcium, and cellular debris within the intima of the walls of large and medium size arteries
Major risk factors for atherosclerosis include[3]
-
Aging
-
Antioxidant insufficiency
-
Chronic inflammation
-
Elevated homocysteine
-
Lifestyle factors (sedentary, Western-style diet, obesity, smoking, pollution)
-
Oxidative stress

Source: Upadhyay, Ravi Kant. “Emerging risk biomarkers in cardiovascular diseases and disorders.” Journal of lipids vol. 2015 (2015): 971453. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Continued exposure to cardiovascular risk factors is mirrored in pathological changes to blood vessels. Loss of integrity of the vascular endothelium is accompanied by atherosclerosis, increased smooth muscle cell migration and proliferation, leukocyte migration, and adhesion.[4]

Progression from risk factors to atherosclerosis and cardiovascular disease mediated by oxidative stress and endothelial dysfunction. The early detection of endothelial dysfunction is a critical point in the prevention of atherosclerosis and cardiovascular disease because this dysfunction could be an initial reversible step in the process of atherosclerosis.
Source: Park, Kyoung-Ha, and Woo Jung Park. “Endothelial Dysfunction: Clinical Implications in Cardiovascular Disease and Therapeutic Approaches.” Journal of Korean medical science vol. 30,9 (2015): 1213-25. This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
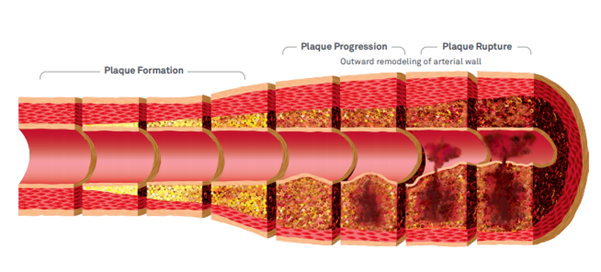
Source: Quest Diagnostics -- https://www.questdiagnostics.com/dms/Documents/Other/CardioIQ_MD46_Brochure.pdf
Early in vivo research demonstrated that atherosclerotic coronary arteries did not dilate in the presence of vasoactive acetylcholine but constricted instead.[5] Endothelial dysfunction continues its rampage even in advanced atherosclerosis as it can promote the rupture of atherosclerotic plaque.[6]
Summary of endothelial dysfunction, atherosclerosis, and CVD
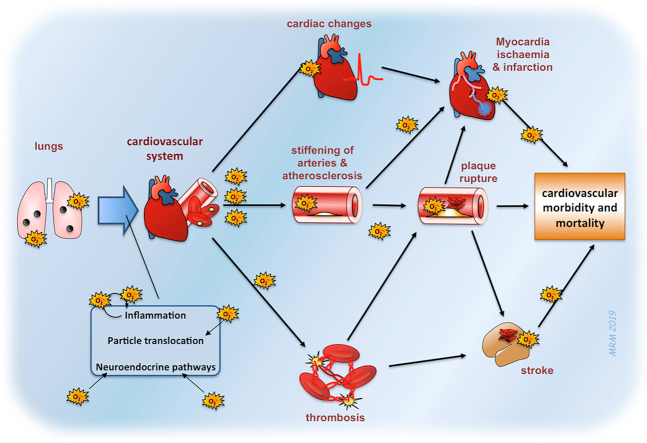
Source: Miller, Mark R. “Oxidative stress and the cardiovascular effects of air pollution.” Free radical biology & medicine vol. 151 (2020): 69-87. This is an open access article under the CC BY license
Pollution and particulate matter contribute to endothelial dysfunction.[7]
- Endothelial dysfunction is an early initiating event in the vascular disease atherosclerosis. Loss of endothelial function and expression of adhesion molecules attracts and tethers circulating inflammatory cells to the vascular wall.
- Additionally, loss of NO and changes to endothelial cell phenotype encourage the oxidation of circulating lipids (e.g., low density lipoprotein (LDL) to oxidized LDL (oxLDL)) that are preferentially retained by inflammatory cells that begin to penetrate the damaged endothelial layer.
- The accumulation of both of inflammatory cells and lipids induces the formation of a fatty plaque in major arteries that grow into the lumen to impede blood flow. Erosion or rupture of advanced plaques is the trigger for thrombosis (a blood clot) that may occlude arteries causing a cardiovascular event such as a heart attack or stroke.
NEXT UP - Endothelial Dysfunction - Assessment Part 1
References[1] Widmer, R Jay, and Amir Lerman. “Endothelial dysfunction and cardiovascular disease.” Global cardiology science & practice vol. 2014,3 291-308. 16 Oct. 2014.
[2] Upadhyay, Ravi Kant. “Emerging risk biomarkers in cardiovascular diseases and disorders.” Journal of lipids vol. 2015 (2015): 971453.
[3] Félétou, Michel. The Endothelium: Part 1: Multiple Functions of the Endothelial Cells—Focus on Endothelium-Derived Vasoactive Mediators. Morgan & Claypool Life Sciences, 2011.
[4] Park, Kyoung-Ha, and Woo Jung Park. “Endothelial Dysfunction: Clinical Implications in Cardiovascular Disease and Therapeutic Approaches.” Journal of Korean medical science vol. 30,9 (2015): 1213-25.
[5] Barthelmes, Jens et al. “Endothelial dysfunction in cardiovascular disease and Flammer syndrome-similarities and differences.” The EPMA journal vol. 8,2 99-109. 6 Jun. 2017.
[6] Barthelmes, Jens et al. “Endothelial dysfunction in cardiovascular disease and Flammer syndrome-similarities and differences.” The EPMA journal vol. 8,2 99-109. 6 Jun. 2017.
[7] Miller, Mark R. “Oxidative stress and the cardiovascular effects of air pollution.” Free radical biology & medicine vol. 151 (2020): 69-87.

